 Not every 911 call is a true emergency. When non-emergency cases occupy first response vehicles, dispatch center call lines, and ER waiting rooms, emergency response systems throughout the US become unnecessarily burdened.
Not every 911 call is a true emergency. When non-emergency cases occupy first response vehicles, dispatch center call lines, and ER waiting rooms, emergency response systems throughout the US become unnecessarily burdened.
These cases divert responders and critical equipment away from the real emergencies, wasting time, resources, and potentially delaying care for those who need it most.
Traditionally, in non-emergency and non-urgent cases, the most immediate point of care has been the emergency department at the nearest hospital. The method of transportation has almost always been an ambulance.
However, a significant portion of EMS patient complaints are more suited to primary care than emergency care. These include:
- Minor headache
- Mild nausea
- Chronic joint pain
- Insomnia
- Minor sprains and strains
In most jurisdictions, EMS providers have no choice but to transport low-acuity patients to the ED by ambulance. The Houston Fire Department (HFD) has made a noteworthy break from this costly model by creating choices to optimize care and reduce waste.
In this post, we’ll look at the challenges caused by non-emergency 911 calls and how the Houston Fire Department, in partnership with Greater Houston Healthconnect and J2 Interactive, implemented a revolutionary solution.
The Impact of Non-Emergent 911 Calls
In Houston, the third largest city in America, emergency medical services receive about 800,000 911 calls every year. Of these, as many as 30% are actually low-acuity calls that don’t qualify as true emergencies.
Unnecessary ambulance dispatches for non-emergency cases divert critical resources from patients who need the most attention, literally pulling responders in the wrong direction.
When patients with non-emergent complaints land in the ED, the problem is further compounded by delaying emergency treatment for the patients who actually need it. In a large metropolitan area such as Houston, the costs and inefficiencies create a substantial burden on the community.
ETHAN is Born
Dr. Michael Gonzalez was among those who saw an opportunity to leverage telehealth and health information exchange technology to reduce costs and increase the effectiveness of time-sensitive patient care.
The idea was to use video conferencing to bring certain EMS patients face-to-face with a physician who could perform remote triage to determine whether immediate ambulance transport to the ED is warranted.
This proposal soon evolved into a program: Emergency TeleHealth And Navigation (ETHAN), launched in 2014 as a partnership between the Houston Fire Department, Houston Health Department, and Greater Houston Healthconnect. The collaboration not only provided immediate efficiency gains among Houston EDs, but also helped identify and prevent frequent misuse of 911 by individuals who are better served in other settings.
How ETHAN Works
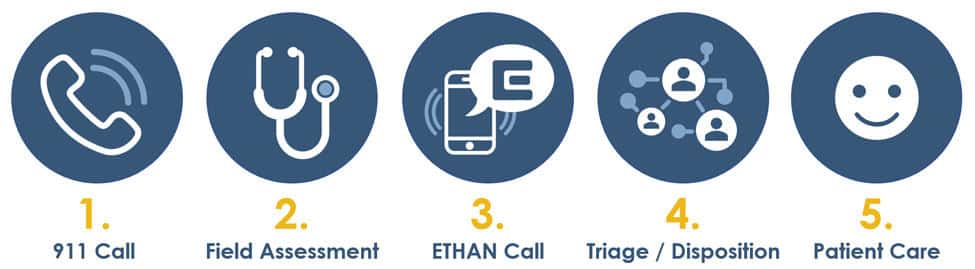
The sequence of the ETHAN process is as follows:
- A 911 call is received by HFD and an ambulance is deployed to the emergency.
- A field assessment by EMS determines whether the case is ETHAN-eligible.
- The on-call HFD physician conducts a live telehealth consultation session, activated via tablet from the field.
- The HFD physician triages the patient and determines an appropriate disposition.
- The patient is scheduled for care, either in the ED, an outpatient clinic, or another setting—potentially transported by taxi instead of ambulance.
The field assessment is the critical step at which the EMS crew determines whether a patient is a candidate for transport, non-transport, or an ETHAN case. Criteria for potential inclusion in the ETHAN program include:
Guidelines for potential inclusion in the ETHAN program are:
- No obvious emergency present
- Ability to speak to physician (or a legally authorized representative present)
- Adult patient with capacity to make decisions
- Pediatric patient with a legally authorized representative present
- Vital signs within reasonable limits
- Ability to care for self
- Ambulatory or a self-propelled wheelchair to reach a taxi
Conversely, exclusion criteria include altered mental status, inability to stand or walk, and acute abdominal pain.
Guided by these criteria, the on-scene EMTs are empowered to make a decision as to whether the patient should be connected to a physician via video call.
As HFD Medical Director David Persse, MD, FACEP points out in this video, there is an element of common sense decision-making before an ETHAN call is initiated. For example, an EMT would know that a taxi driver is not going to want to take a patient who is clearly in a lot of pain or distress, even if their symptoms aren’t caused by a serious medical illness. These types of conditions could cause the attending EMT not to initiate an ETHAN consultation.
Telehealth Infrastructure
The telehealth capability at the heart of the ETHAN solution rests on a number of key components that continue to evolve and improve as ETHAN matures.
Field Computers
HFD ambulances are equipped with electronic tablets for functions such as dispatch, documentation, and video conferencing between emergency responders, the patient, and a call center physician.
Panasonic’s TOUGHPAD was selected to serve as the field computer hardware device. The HFD is moving to the TOUGHBOOK, which adds a keyboard and other capabilities.

Volunteer physicians in Houston’s 911 call center communicate directly with patients via video conference, an evaluation that is analogous to a face-to-face encounter in a hospital emergency department.
While the video encounter takes place, the field crew remains available to assist the physician by collecting other important information from the patient.
Teleconferencing
Cisco Telepresence is used for HIPAA-compliant video conferencing. Local integrator DataVox worked with HFD to embed video conferencing capability.
Wireless Coverage
Comprehensive wireless coverage and data transmission speed are crucial for real-time physician and patient interactions. The ETHAN team selected the Verizon Wireless 4G LTE network for communication.
This enables the physician to remotely view cues such as facial expressions or the patient physically indicating where they feel pain.
Verizon’s network team was directly involved in testing the coverage area.
The Role of Greater Houston Healthconnect
Greater Houston Healthconnect (GHH), a non-profit health information exchange (HIE) serving 24 counties in Southeast Texas, provides the patient data and information pipeline that powers the ETHAN platform.
GHH also administers the program, maintaining partnerships with care centers, transport companies, and other key stakeholders involved in coordinating appropriate levels of care for residents and visitors of the Houston metro area.
On the technical side, GHH:
- Provides the HIE infrastructure that makes triage and care coordination possible
- Delivers patient history seamlessly within the consulting physician’s native EHR
- Develops and hosts the application software that drives the ETHAN workflow
“Greater Houston Healthconnect has been an integral part of ETHAN from program inception—and they have been a key partner in developing and expanding ETHAN operations, as we continue to improve and upgrade our mobile health capabilities.”
Project Director, ETHAN Program
Since the ETHAN workflow involves non-EMS transport and point of care settings other than the ED, the process needed to integrate additional systems and services. With a more robust and streamlined portal, on-call physicians can focus on patient care while accessing a single view into the ETHAN process rather than switching between applications.
J2 Interactive collaborated with GHH to develop the following essential ETHAN components:
- Greater Houston Healthconnect’s health information exchange, built on the InterSystems HealthShare platform, which connects an extensive network of care providers throughout the region
- An appointment scheduling system for participating clinics
- Transportation booking through local taxi services
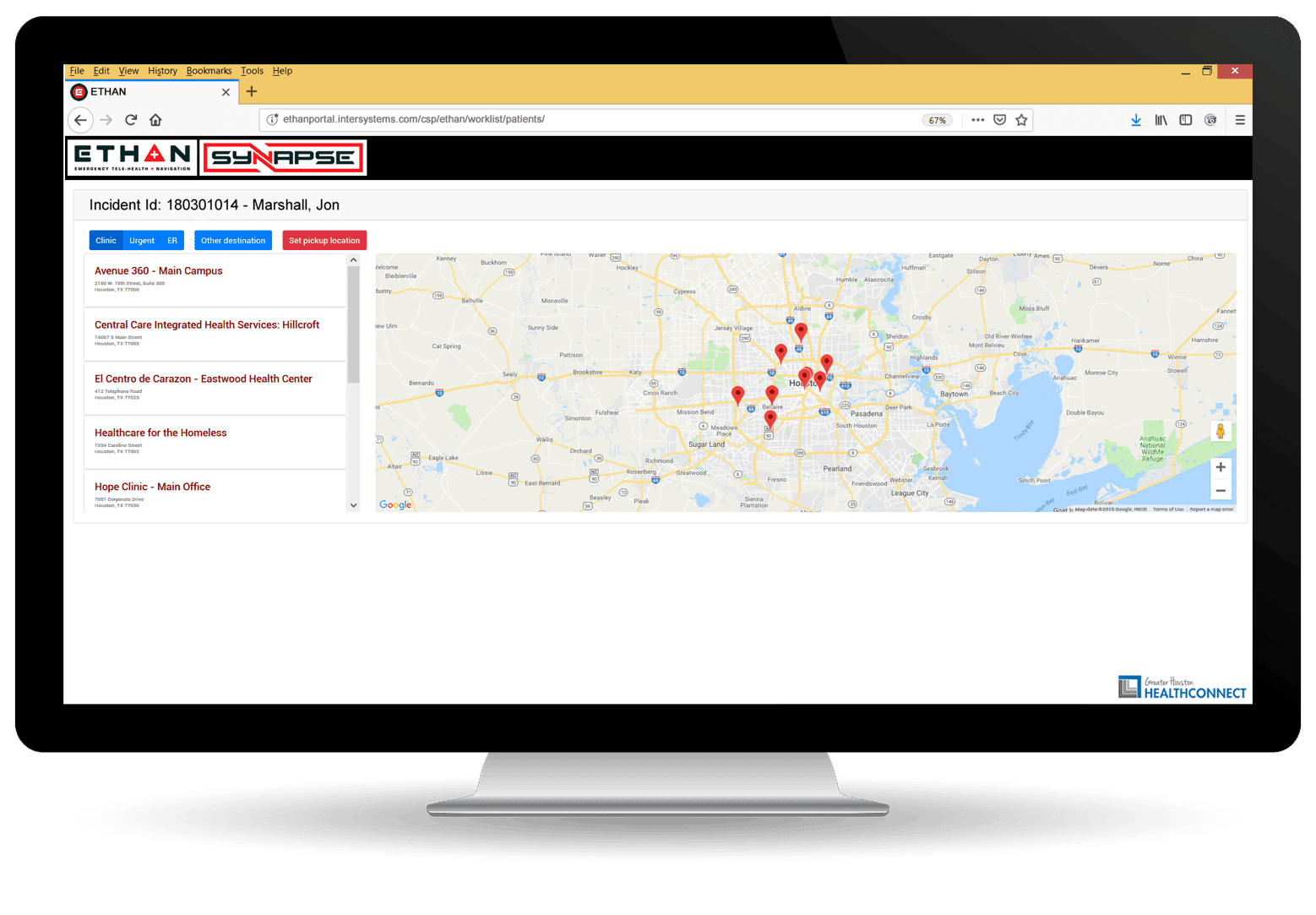
The screenshot below shows the ETHAN facility locator, part of the ETHAN portal built by J2 and GHH on the HealthShare platform:
The Results
The ETHAN program has provided a number of tangible benefits to the City of Houston by transforming the way the Houston Fire Department handles non-emergency 911 calls.
Improved Resource Utilization
The deflection to alternate means of transportation has the important benefit of putting HFD ambulances back in service faster. 89% of patients selected into the ETHAN program use alternate transportation to the ED (taxi or self-transport). The cost of a cab ride is approximately 2% of the cost of an ambulance transport.
According to the Western Journal of Emergency Medicine, “Median time from EMS notification to unit back in service was 44 minutes [53%] faster for the ETHAN group” as compared to a control group.
With ETHAN, the average time between a 911 call and a patient arriving at the point of care (ED or clinic) has gone from 71 minutes to a remarkable 33 minutes.
ED Visit Avoidance
Thanks to the remote triage enabled by the program, 13% of ETHAN patients avoid ED visits altogether. This reduces the total number of patients that need to be treated in the emergency setting. The cost of a clinic visit is approximately 15% of the cost of an ED visit.
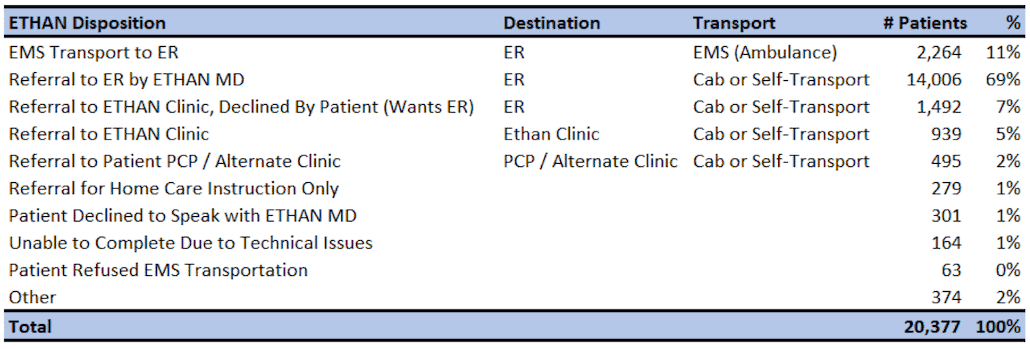
The table below shows the full breakdown of ETHAN dispositions for the first four years of the program (December 2014 through October 2018).
ETHAN dispositions from December 16, 2014 – October 28, 2018, provided by HFD

Cost Savings
In addition to its impact on quality of care and patient outcomes, ETHAN has delivered extraordinary financial benefits. On average, a typical ambulance ride ($1,000) and ED visit ($1,200) costs a total of $2,200. But if an ETHAN encounter results in a $20 taxi ride to the ED, that’s a cost reduction of $980. If instead the ETHAN consulting physician recommends a taxi to an appointment at an outpatient clinic instead of an ED visit via ambulance, the savings is $1,980!

In the following presentation from the 2019 HIMSS conference, Nick Bonvino (CEO of Greater Houston Healthconnect) and Lou LaRocca (President and CEO of J2 Interactive) describe the ETHAN use case and discuss the time and resource savings that the project has already realized.
Looking Forward
With the help of GHH and J2, the ETHAN program continues to evolve and innovate for the people of Houston, with regular updates that extend its reach and capability.
In the meantime, ETHAN provides a dynamic and effective model for other healthcare facilities and fire departments that are looking to reduce the cost of non-emergency 911 calls and preserve emergency system resources for the patients who truly need it.
Want to learn more? Drop us a line below.
About J2 Interactive
 J2 Interactive is an award-winning software development and IT consulting firm specializing in customized solutions for hospitals, labs, research institutions, and health information exchanges.
J2 Interactive is an award-winning software development and IT consulting firm specializing in customized solutions for hospitals, labs, research institutions, and health information exchanges.
Our approach to design and development is rooted in a fundamental belief that systems succeed or fail based on how well they serve the people who depend upon them.

