| Day One Summary | Day Two Summary | Day Three Summary |
|---|
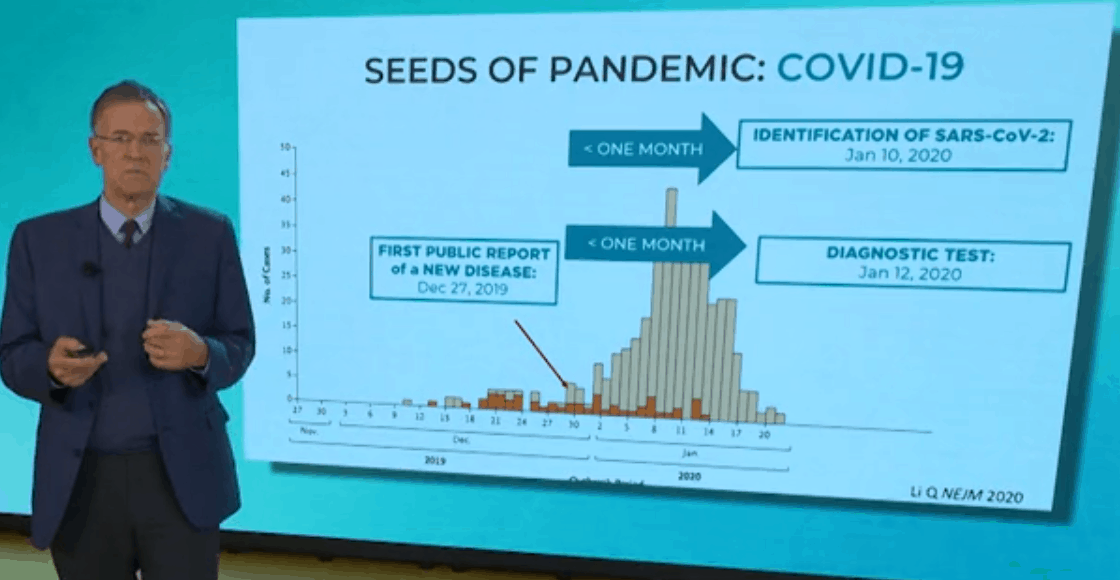
2020 marks the first year ever of InterSystems’ Global Summit going virtual! Join us from October 20th to November 5th as we recap various sessions of this year’s event.
Welcome, by InterSystems Executives

- Date: October 20, 2020
- Presenter: Paul Grabscheid, VP of Strategic Planning, InterSystems
- Overview: Paul Grabscheid welcomed viewers and opened the first-ever Virtual Summit.
Paul Grabscheid, VP of Strategic Planning for InterSystems, welcomed viewers and opened the first-ever Virtual Summit with a brief overview of InterSystems as a company, highlighting its three major products:
- InterSystems IRIS, which delivers high-performance database management, interoperability, and analytics platform
- InterSystems HealthShare Family of Products, including:
- HealthShare Unified Care Record
- HealthShare Personal Community
- HealthShare Health Insight
- HealthShare Patient Index
- HealthShare Provider Directory
- HealthShare Health Connect
- InterSystems TrakCare, a unified healthcare information system
Mr. Grabscheid introduced each of the Virtual Summit keynote presenters and thanked viewers for attending this year’s events.
- Terry Ragon, CEO & Founder, InterSystems
- Gregg Meyer, MD, MSc, Chief Clinical Officer, Mass General Brigham
- Fiona Murray, AM, PhD, Associate Dean for Innovation and Inclusion, MIT Sloan School of Management
- Bruce Walker, MD, founding director, Ragon Institute of MGH, MIT, and Harvard
- John Paladino, Head of Client Services, InterSystems
- Paul Tibbits, MD, Executive Director, Office of Technical Integration, VA
- Don Woodlock, Head of Healthcare Solutions, InterSystems
- Michael B Marchant, Director, Health Information Exchange & System Integration, UC Davis
- Lloyd McCann, MHB, MBChB, MHSM CEO, Mercy Radiology and Clinics.
- Scott Gnau, Head of Data Platforms, InterSystems
- Jittu Lulla, Wealth Architect, Broadridge
- Marinela Tudoran, Managing Director, Credit Suisse
- Alexandre Conceição, CIO, BBTS
- Dimitri Fane, Director, TrakCare Product Management, InterSystems
- Dimitri Fane, Director, TrJonathan Teich, MD, Director, HealthShare Product Management, InterSystemskCare Product Management, InterSystems
- Jeff Fried, Director, Data Platforms Product Management, InterSystems
Adapt and Thrive in a Changing Environment

- Date: October 20, 2020
- Presenter: Terry Ragon, CEO & Founder, InterSystems
- Overview: InterSystems Founder and CEO, Terry Ragon, discussed ways to innovate and improve a crisis situation.
Terry Ragon, InterSystems Founder & CEO, provided viewers with an encouraging message: look at a crisis situation as an opportunity to innovate and improve. Ragon discussed how some organizations have matured to a state where following prescribed processes is their goal mark of success. Such an approach can lead to rigidity and stagnation. In fact, as Ragon pointed out, the most successful organizations resist the temptation to settle into a process-driven culture and instead maintain a strong vision and objectives-driven culture.
 In these successful organizations, their assets and energy are aligned to achieve something of value outside of the company itself, allowing them to find success in a rapidly changing and uncertain environment. Ragon described a test for determining the risk of a process-driven culture in an organization. First, go down your organization. At what point is following the company’s process the goal of a person’s job? The closer to the top this phenomenon occurs, the higher the risk that the organization might be falling prey to a less flexible or agile process-bound culture.
In these successful organizations, their assets and energy are aligned to achieve something of value outside of the company itself, allowing them to find success in a rapidly changing and uncertain environment. Ragon described a test for determining the risk of a process-driven culture in an organization. First, go down your organization. At what point is following the company’s process the goal of a person’s job? The closer to the top this phenomenon occurs, the higher the risk that the organization might be falling prey to a less flexible or agile process-bound culture.
Ragon stressed how InterSystems continues to stay committed to improving the health of populations around the world and remaining flexible. Doing so often means being willing to adapt, substitute, experiment, and learn from others. It is exactly that flexibility that fosters innovation and leads to value.
To close, Ragon officially welcomed attendees to this year’s Virtual Summit, thanked current customers, and stated how he looks forward to meeting and working with those who are considering InterSystems solutions today.
Turning on a Dime: Mass General Brigham and COVID-19

- Date: October 20, 2020
- Presenter: Gregg Meyer, MD, MSc, Chief Clinical Officer, Mass General Brigham
- Overview: Dr. Gregg Meyer’s presentation described Mass General Brigham’s experience in rapidly responding to COVID-19 this year.
Dr. Meyer, the Chief Clinical Officer for Mass General Brigham (MGB) and Professor of Medicine at Massachusetts General Hospital and Harvard Medical School, explained that many large organizations often struggle with agility and speed. MGB is part of the largest non-governmental employer organizations in Massachusetts and is the largest hospital-based research organization in the country. An organization of this size faces a considerable amount of stress when things move quickly. Dr. Meyer likens rapid responses to environmental changes as trying to turn an aircraft carrier on a dime. The task is daunting.
 Prior to the emergence of COVID-19, MGB had an emergency command center and leadership structure in place to respond to the then-current national shortage of sterile gowns. As COVID-19 began to make itself known, MGB’s emergency operations center shifted its focus from sterile gowns to understanding and organizing response and mitigation efforts related to this virus. Having this command center structure in place and actively functioning was key to MGB’s ability to mobilize and respond more quickly than it might have otherwise.
Prior to the emergence of COVID-19, MGB had an emergency command center and leadership structure in place to respond to the then-current national shortage of sterile gowns. As COVID-19 began to make itself known, MGB’s emergency operations center shifted its focus from sterile gowns to understanding and organizing response and mitigation efforts related to this virus. Having this command center structure in place and actively functioning was key to MGB’s ability to mobilize and respond more quickly than it might have otherwise.
MGB identified a list of critical needs as it worked through growing COVID-19 concerns and public health implications. They needed:
-
- More enterprise analytics to track diagnoses, geo-mapping, workforce, and supply chain
- An enterprise-wide bed availability command center and an ability to track surge capacity
- Clearer decision rights in the command center with escalation pathways
- A trained support resource for respite and/or substitution for each member of the Incident Command System and command center
- A single repository of HR and Occupational Health data to assess workforce capacity
- A catalog of skills possessed by the workforce that could be used in a crisis, even if not part of their regular job
- Points of contact for key stakeholders such as the Department of Homeland Security and Department of Defense
- Knowledge of the source of their supply chain and redundancy options for key products necessary to respond to an emergency
- Settlement on a single collaboration tool and get everyone trained to use it effectively
- A quick stand-up intelligence-gathering unit
- A system-wide ethics group
MGB was ultimately able to respond much more quickly than expected, including implementing a new telehealth solution scheduled to take two years to deploy in a matter of weeks. Other solutions they implemented include rapidly developed COVID-19 dashboards and tools to identify where COVID-19 positive patients originated/additional critical information about them that aided in treatment and community and partner outreach efforts. The overall MGB response even included developing solutions to help family members say goodbye to loved ones remotely and as meaningfully as possible. Dr. Meyer credited the following list of factors in MBG’s ability to “turn the ship” much faster than many would have thought possible:
- Public acknowledgment of the possibility of the situation, flexibility and commitment to listening/learning from others, and collaborative disposition
- Enablement of leaders to be able to make quick decisions about what kind of work is most important and should receive time and attention and what kind of work can be suspended
- Willingness to give those without all of the usual credentials the opportunity to step up and take responsibility or re-assign elsewhere if needed
- Professionally ignoring and moving past those within the organization who said that something couldn’t be done
- Encouragement of flexibility and active feedback/discourse
- Recognition of signs of stress and burnout among staff and implementing measures to take care of them
- Having their leaders ignore outside distractions, focusing on the issue at hand with all of their energy
Dr. Meyer explained that MGB did not do much that was truly different or new but instead had a strong enough resolve and motivation to make quick, firm decisions to remove the many distractions that tend to slow down a given response.
 Dr. Meyer ended his presentation by sharing his view that a lot of work remains, and there will certainly be other threats in the future that they will be ready to handle. There will likely be a long tail to COVID-19, and healthcare professionals should be ready for a long journey with it and future public health emergencies. His key takeaway: “Optimism is a force multiplier.” Remain positive and continue to focus on the most valuable work, distraction-free.
Dr. Meyer ended his presentation by sharing his view that a lot of work remains, and there will certainly be other threats in the future that they will be ready to handle. There will likely be a long tail to COVID-19, and healthcare professionals should be ready for a long journey with it and future public health emergencies. His key takeaway: “Optimism is a force multiplier.” Remain positive and continue to focus on the most valuable work, distraction-free.
Innovation and Adaptation: Building a Resilient Organization

- Date: October 20, 2020
- Presenter: Fiona Murray, AM, PhD, Associate Dean for Innovation and Inclusion, MIT Sloan School of Management
- Overview: Dr. Murray gave guidance for leaders as they consider streamlining and preparing their organizations to navigate change and disruption, based on her research at MIT and experience gained during the COVID-19 pandemic.
Dr. Fiona Murray, MIT Sloan School of Management’s Associate Dean for Innovation and Inclusion, began her session with an overview of MIT’s concept of innovation. At MIT, innovation is “the process of taking ideas from inception to impact.” For their purposes, an idea is a match between a problem and a solution, and the idea’s impact ought to have some value beyond simply profit.
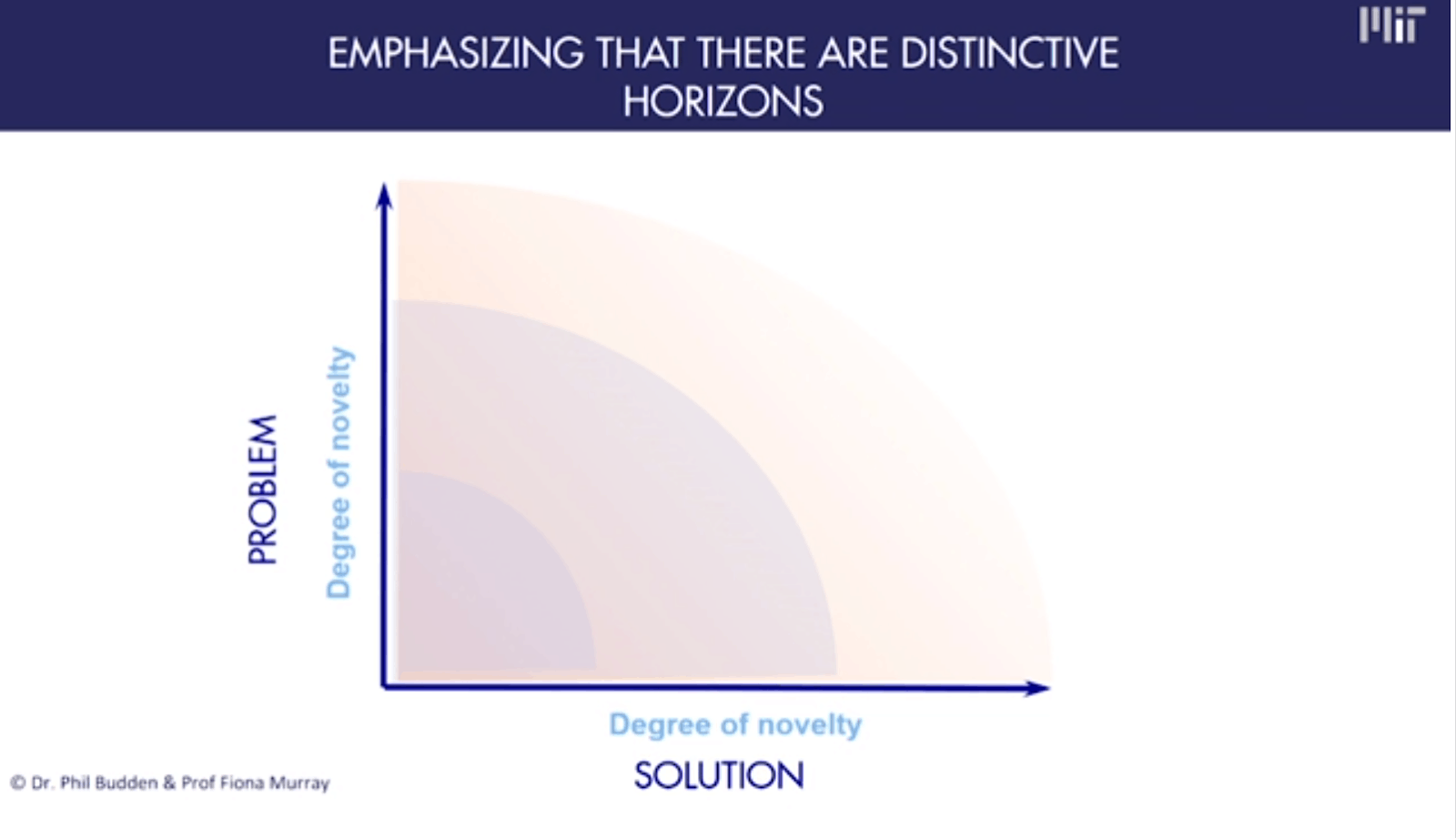 Moving from inception to impact is considered a journey, and it is that process that is the focus of Dr. Murray and the MIT community. Dr. Murray presented a graph to articulate where organizations might find themselves and what kind of innovation journey they are on. The graph showed Problems on the vertical axis and Solutions plotted along the horizontal axis. The concept is that the more complex a problem is and the most complex a solution is, the organization finds itself needing to exist in increasingly risky spaces of exploration and hypothesizing. If a problem is less complex, and the solution is somewhat more pedestrian, an organization is likely doing the normal day-to-day work of incremental innovation.
Moving from inception to impact is considered a journey, and it is that process that is the focus of Dr. Murray and the MIT community. Dr. Murray presented a graph to articulate where organizations might find themselves and what kind of innovation journey they are on. The graph showed Problems on the vertical axis and Solutions plotted along the horizontal axis. The concept is that the more complex a problem is and the most complex a solution is, the organization finds itself needing to exist in increasingly risky spaces of exploration and hypothesizing. If a problem is less complex, and the solution is somewhat more pedestrian, an organization is likely doing the normal day-to-day work of incremental innovation.
According to Dr. Murray, if we are to be adaptive, flexible, and best handle shocks such as COVID-19, we must spend our time exploring new horizons. That begins with having a strategic vision that encourages and supports risk-taking in complex environments. We might see the hallmarks of these types of organizations in start-up companies, for example. Start-ups are geared to explore, iterate, move quickly, and take certain risks that other, more mature, organizations might not. It is the organization’s ability to rapidly seek new solutions and pivot quickly that positions it to survive and even thrive in disruptive environments. Some companies have completely shifted their focus to accelerate innovations tied to COVID-19 to become part of the eventual solution.
 Dr. Murray distilled much of the knowledge and insight from available business and management books into the following key ideas:
Dr. Murray distilled much of the knowledge and insight from available business and management books into the following key ideas:
- Most effective teams and organizations use rapid, iterative innovation loops.
- There are two main features of these loops: Experimentation and Evaluation.
- Experimentation and evaluation loops are as small, fast, and inexpensive as possible.
The most successful organizations are able to use these approaches while focusing on the most important problems to solve. Put another way; they are able to prioritize sufficiently well to stop work on projects or tasks that are not directly related to the highest-value work.
Dr. Murray provided the following guidance for leaders as they consider streamlining their organizations and preparing to navigate change and disruption:
- Establish a clear strategic direction that can enable leaders to make quick decisions about prioritization and non-essential work.
- Enable a system that rewards and supports experimentation, learning, and evaluation.
- Ensure a diverse network from which to hear and harness ideas, given the evidence showing the strength and range of successful innovations among diversely connected organizations.
Dr. Murray concluded her session by encouraging viewers to reflect on their ability to influence these three key elements in their own organizations.
The Quest for a COVID-19 Vaccine and the Need for Agility in Life Sciences

- Date: October 20, 2020
- Presenter: Bruce Walker, MD, founding director, Ragon Institute of MGH, MIT, and Harvard
- Special Introduction: Dr. Anthony Fauci, Director, National Institute of Allergy and Infectious Diseases
- Overview: Dr. Bruce discussed the history of his work on HIV, how that connects to the Ragon Institute’s current research on COVID-19, and the impact of that research.
 Opening the presentation was Dr. Anthony Fauci, who has known Dr. Bruce Walker for over 30 years. When they first met, Walker was a young physician-scientist in the middle of working with and identifying an emerging and perplexing disease that would later become known as HIV, the virus that causes AIDS. Walker was among those on the front lines of researching and attempting to solve the problems caused by this disease.
Opening the presentation was Dr. Anthony Fauci, who has known Dr. Bruce Walker for over 30 years. When they first met, Walker was a young physician-scientist in the middle of working with and identifying an emerging and perplexing disease that would later become known as HIV, the virus that causes AIDS. Walker was among those on the front lines of researching and attempting to solve the problems caused by this disease.
The Ragon Institute’s mission is to harness the human immune system to cure the most formidable diseases around the world, including Ebola, Zika, and HIV. Dr. Fauci acknowledged Terry and Susan Ragon’s generous funding to support this work.
Science will be front and center in both ending the COVID-19 pandemic and preventing and curing diseases of the future. These solutions will be achieved through collaboration, research, and rapid adaptation, initiatives the Ragon Institute continues to support. Today’s closing speaker, Bruce Walker, is its founding director.
 Dr. Walker opened his session with the history of his work on HIV, including the troubling death rate among those affected as well as the promise of coming across patients whose own immune systems seemed to keep the virus at bay for many years, and the prospect of a vaccine or cure. Dr. Walker’s work took him to Africa, where he had the opportunity to help build one of the first African research establishments focused on understanding this virus and the human body’s ability to respond to it.
Dr. Walker opened his session with the history of his work on HIV, including the troubling death rate among those affected as well as the promise of coming across patients whose own immune systems seemed to keep the virus at bay for many years, and the prospect of a vaccine or cure. Dr. Walker’s work took him to Africa, where he had the opportunity to help build one of the first African research establishments focused on understanding this virus and the human body’s ability to respond to it.
Dr. Walker presented a series of illustrations to explain viral and bacterial pathogenesis mechanisms, highlighting that viruses exist with scant genetic material but still overpower our responses and commandeer our genetic material for their own purposes. The presentation included a summary of how SARS-COV-2 causes an “inflammatory storm” and affects oxygen transfer in the body.
One of the features that makes COVID-19 more aggressive for many and riskier from the public health perspective is that the result of infection is a weakened, damaged antibody response. Damaged antibodies do not have the same durability that a normal immune response might have, leading to less chance for long-term immunity.
Dr. Walker described the quick response from the global community to find a treatment or vaccine for COVID-19. It was during a semester of teaching a course on epidemics that he, his students, and colleagues first started to hear stories about a flu-like illness in Wuhan. The course he was teaching suddenly took a more urgent turn to focus on this new emerging outbreak. Dr. Walker realized that the Ragon Institute would need to make that same pivot. Today, it focuses on supporting COVID-19 research.
Dr. Walker described a number of the most common approaches to developing vaccines and mentioned the progress that researchers are now making to find a safe, effective, scalable, and durable vaccine. Walker ended his session with the following conclusions:
- The scientific community is leveraging what they have learned from other diseases and vaccine programs to find shorter paths to solutions; COVID-19 vaccine research is moving at an unprecedented rate given what has been learned in the past about HIV and other pathogens.
- The ability to pivot quickly is essential to success, both longer-term, but especially during emergencies as conditions and information change rapidly.
- Vaccines for COVID-19 will likely be available (at least on some level) as early as late 2020
- Vaccines will be more widely available by the second half of 2021.
- Multiple successful vaccines will certainly be needed to meet global demand to treat potentially billions of people.
- In the meantime… wear masks! Front-line healthcare workers spend entire shifts with COVID-19 positive individuals and yet do not contract the virus themselves. When used properly, masks work!
| Day One Summary | Day Two Summary | Day Three Summary |
|---|
![]()
Thank you for joining us for today’s recap. J2 has been a trusted InterSystems Implementation Partner since 2004. Learn more about us and our involvement in InterSystems Virtual Summit 2020.
J2 Interactive is an award-winning software development and IT consulting firm with projects ranging from technology strategy and best-practices consulting to systems integration, application development, health information exchange, and business intelligence.
J2 is a recognized leader in interoperability solutions for customers of all sizes. Drop us a line to find out why.

