Part 1
 Recent CMS and ONC rulings will make SMART on FHIR capabilities within an EHR mandatory. This capability provides a consolidated view of patient progress over time in ways that have not been possible until recently. Before reading about what these rulings mean for you and your healthcare organization, you might be wondering what is FHIR and what is SMART? More importantly, what happens when you put the two together?
Recent CMS and ONC rulings will make SMART on FHIR capabilities within an EHR mandatory. This capability provides a consolidated view of patient progress over time in ways that have not been possible until recently. Before reading about what these rulings mean for you and your healthcare organization, you might be wondering what is FHIR and what is SMART? More importantly, what happens when you put the two together?
In Part 1, we will answer those questions and discuss the reasons behind SMART on FHIR’s conception. In Part 2, we have compiled all the important information you need to know about the CMS and ONC rulings.
(Part 1 | Part 2)
SMART on FHIR has developers across the continuum of care excited like never before. Why? Because the biggest EHRs in the industry work with SMART on FHIR apps. This means that widgets you build in-house will be compatible with Epic, Cerner, and other major players. Over the past few years, J2 has collaborated with organizations to release several SMART on FHIR applications on the InterSystems HealthShare and Salesforce Health Cloud platforms. How can this technology benefit your organization?
Why SMART on FHIR?
At many health systems, workflows span not only different areas of an EHR but also a variety of applications and software across various physical locations. The progression of a patient over time cannot be easily viewed in one place by a caregiver.
A physician may need to log into different healthcare applications to get a complete view of a patient’s treatment and progress over time, or a doctor may have to task a staff member with manually assembling workflows. These processes take time and have an internal cost.
Let’s go to a popular example and track the progress of premature infants. When a baby is born prematurely, the initial care provided at the hospital represents one track in the overall care for the patient. The next visit could be at an outpatient office (in the same or a different healthcare system) representing a separate workflow, and subsequent appointments or hospital stays also mean additional tracks in that ongoing continuum of care.
With SMART on FHIR, this disparate data can be assembled in a longitudinal view so that caregivers no longer need to switch among different applications to piece together a complete patient story. With the unification of underlying data, a host of possibilities are unlocked. For example, applications can display graphs to offer a comprehensive visualization of patient progress. In the case of the premature infant, the visualization can display key health indicators such as length, weight, and head circumference—over time and across different caregivers and facilities.
[layerslider id=”6″]FHIR enables caregivers to view a complete patient record, which can be presented in multiple ways. Source: Boston Children’s Hospital SMART on FHIR Growth Chart
An overview of FHIR
Initially released in 2014, FHIR (a set of standards, FHIR meaning Fast Healthcare Interoperability Resources) was a response to the need for a more contemporary standard for the exchange of information in healthcare environments.
FHIR is published by Health Level Seven International (HL7), the same HL7 that has set the gold standard for healthcare IT interoperability formats for decades. They are an ANSI-accredited standards developing organization that provides a framework for the exchange, integration, sharing, and retrieval of electronic health information that supports clinical practices and health services.
On the technical side, FHIR is an evolving set of standardized APIs among different healthcare resources. Some examples of these resources are:
- Patient
- Practitioner
- Location
- Appointment
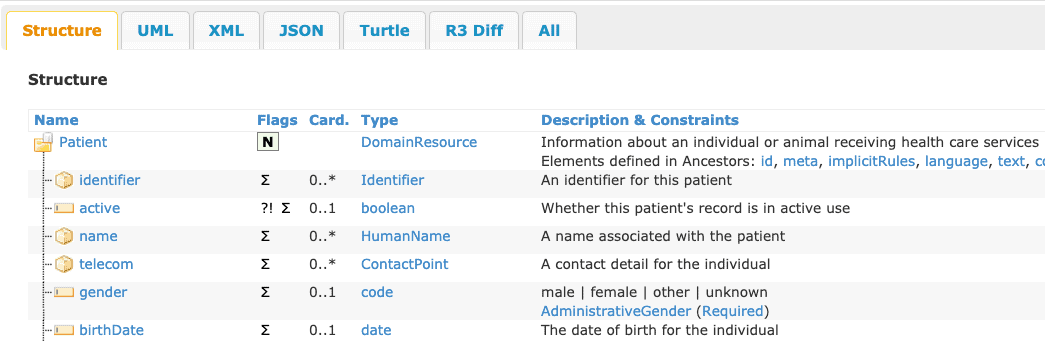
Each resource has a detailed definition. If you’re technically-minded, here is part of the specification for the Patient Resource, which is the “who” information about a patient.
Because FHIR is still evolving, the many resources (there are over 150) are at varying levels of stability and implementation readiness.
At a high level, FHIR defines data structure in addition to securely retrieving and presenting the data in an EHR and other interfaces.
An overview of SMART
SMART (Substitutable Medical Applications and Reusable Technologies) is a standards-based, interoperable apps platform for electronic health records.
SMART was originally developed—before FHIR was ever ignited—by the Harvard Medical School and Boston Children’s Hospital in 2010. It began an interoperability project with the distinctive goal of developing a platform to enable medical applications to be written once and run unmodified across different healthcare IT systems.
In addition to health systems providers, SMART has applicability for patients. For example, veterans can now access their health records using Apple’s SMART on FHIR health app.
How SMART and FHIR come together
In 2013, SMART was updated to leverage the FHIR standard. However, that was still early on in the evolution of FHIR.
Today, SMART & FHIR represent an open, standardized, and practical means of exchanging data among EHRs, health system sites, and data sources. The SMART team maintains a sandbox and app gallery and continues to innovate with projects like CDS Hooks, Flat FHIR, and SMART Markers.
What’s next for SMART on FHIR
As of May 2020, the 21st Century Cures Act and Final Rule from the ONC made SMART a certification requirement for Health IT Modules, marking the next step in healthcare interoperability. We are excited by these changes and have compiled the information you need to know about the mandate in part 2 of this article!
What organizations should be most excited about
SMART on FHIR is becoming a requirement for organizations nationwide, providing a compelling reason to roll out a SMART on FHIR capability. There’s more than Federal compliance to get excited about, however. Before, large EHR vendors like Epic and Cerner did not have very open APIs to encourage outside development. Thanks to a cultural shift spurred by the Federal government, apps that are compatible with SMART on FHIR will link right up to previously closed-off (but incredibly popular) EHRs. Want to see for yourself? Check out Cerner’s sandbox.